Vaccination Requirements
Meningococcal vaccination is part of a risk-mitigation strategy that takes into account how C5 inhibitors work1,2
Due to the risk of meningococcal infections, ULTOMIRIS is available only through a restricted program under a Risk Evaluation and Mitigation Strategy (REMS). Enrollment in the REMS program and additional information on the requirements are available at UltSolREMS.com or by calling 1-888-765-4747.
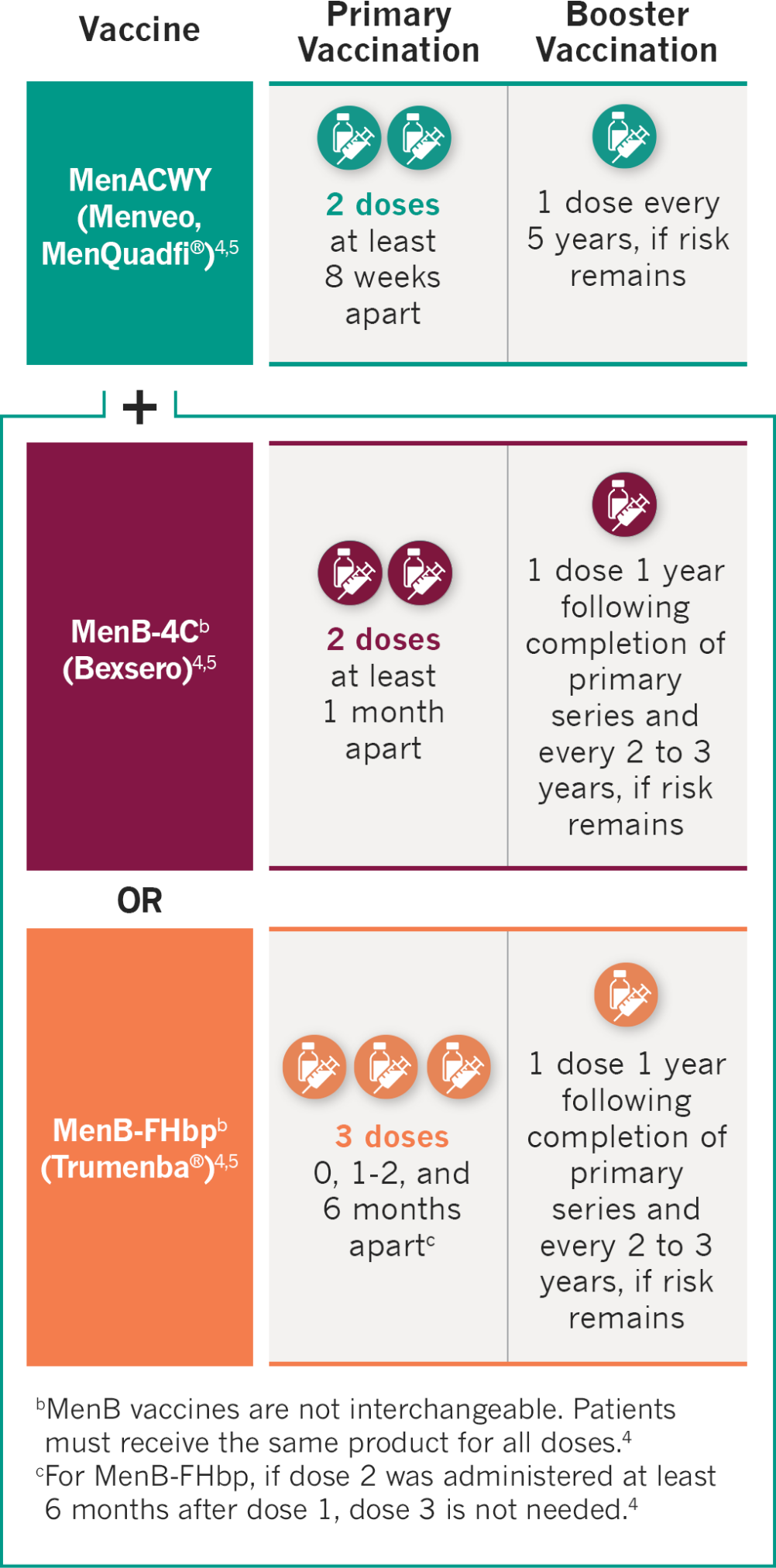
Complete or update meningococcal vaccination (for serogroups A, C, W, Y and B) at least 2 weeks prior to administration of the first dose of ULTOMIRIS, per the current Advisory Committee on Immunization Practices (ACIP) recommendations for patients receiving a complement inhibitor.1
- ACIP recommends that persons using complement inhibitors should be vaccinated at least 2 weeks before complement inhibitor initiation unless the risks for delaying treatment outweigh the risks for developing meningococcal disease.3
- Revaccinate patients in accordance with ACIP recommendations considering the duration of ULTOMIRIS therapy.1,a
aNote that ACIP recommends an administration schedule in patients receiving complement inhibitors that differs from the administration schedule in the vaccine prescribing information.1
If patients have not been vaccinated and ULTOMIRIS must be started right away, antibacterial drug prophylaxis should be administered1,d
dSeveral antibiotics are available for the treatment of meningococcal disease, including ceftriaxone, cefotaxime, and, when the diagnosis is confirmed, penicillin.3
The benefits and risks of antibiotic prophylaxis for prevention of meningococcal infections in patients receiving ULTOMIRIS (ravulizumab-cwvz) have not been established. Various durations and regimens of antibacterial drug prophylaxis have been considered, but the optimal durations and drug regimens for prophylaxis and their efficacy have not been studied in unvaccinated or vaccinated patients receiving complement inhibitors, including ULTOMIRIS. Vaccination does not eliminate the risk of meningococcal infections, despite development of antibodies following vaccination.1
Revaccinate patients in accordance with ACIP recommendations considering the duration of ULTOMIRIS therapy. Note that ACIP recommends an administration schedule in patients receiving complement inhibitors that differs from the vaccine prescribing information.1
Please see the respective meningococcal vaccine’s Prescribing Information for complete details, including the vaccine’s Warnings, Precautions, and Contraindications.
- If your patient received meningococcal vaccines in the past, they might need additional vaccination before starting ULTOMIRIS4
- The choice of vaccine deemed medically appropriate is your independent decision
- In most cases, your patients can receive meningococcal vaccines at a physician’s office or retail pharmacy
- MenACWY and MenB vaccines may be administered during the same visit but at different injection sites6
- To help reduce the risk of meningococcal infections, the complete series for the MenACWY and MenB vaccines should be administered4
Support for your patients and your practice
Discover starter kit materials, dosing instructions, vaccination requirements, patient safety tools, and more.
Explore Resources